MORPHOLOGICAL CHARACTERISTICS
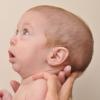
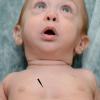
The appearance of newborns with Pierre Robin sequence is typical. They have small lower jaw (micrognathia) and usually cleft palate (in these cases, this typically results in a horseshoe or U-shaped cleft palate).
FREQUENCY – ETIOLOGY
Robin Pierre sequence is a rather uncommon abnormality (it happens once in 8,500 to 14,000 births) and in some cases it may be a part of other syndromes such as Treacher Collins, Stickler, Velocardiofacial syndrome, etc.The root causes are not known, but it is considered that the mechanical factors that limit the fetus might be responsible for the small size of the lower jaw (micrognathia). The lower jaw in turn prevents the tongue of going down in time from the high position that is held in the mouth of the fetus to leave space at the side portions of the palate to develop in the midline and join, resulting to a cleft palate.
HOW IS PIERRE ROBIN SEQUENCE (PRS) DIAGNOSED?
The diagnosis of PRS is made only with the clinical examination of the newborn.
FUNCTIONAL PROBLEMS
The main symptoms of Pierre Robin sequence are the following:
- Breathing difficulties (respiratory problems such as respiratory distress or/and respiratory obstruction)
- Feeding difficulty.
The respiratory distress may be evident only when the newborn has been tired from the effort to breathe, usually in supine position and this can endanger the life of the newborn. A careful follow-up of his/her respiratory function and adequate oxygenation is required.
Because of the small jaw and of respiratory distress, feeding difficulty may occur as well. The follow-up of the newborn must be continuous, especially in the initial stages, because although he/she seems to breathe and be oxygenated sufficiently when he/she is tired or when he/she sleeps signs of respiratory obstruction may appear.
TREATMENT - CONSERVATIVE TREATMENT SUPPORT
All the effort is focused on the support of the respiratory function. Most of the times, the symptoms often improve within a few days or weeks. The newborn should not be placed and remain in supine position when he/she is not under supervision. Often, the placing of the newborn in prone position (face down) it sufficiently ensures better breathing. In more severe cases, the newborn should remain in the intensive care unit, where he/she may be aided by non-invasive means such as by placing of a small tube that holds the tongue forward thereby facilitating the respiration. It’s emphasized again that in most of the cases the symptoms improve within days or weeks. To overcome the feeding difficulty it may be required a placement of a nasogastric tube to ensure receiving adequate nutrition.
SURGICAL TREATMENT
The newborn may need surgery only in those cases where despite the efforts for some time with preservative treatments there is no improvement. The earliest Rutledge surgery that consists of a temporary adhesion of the lower surface of the tongue with the inner surface of the lip (to be held in front of the tongue) has been almost abandoned because of the high rate of failure. It has also been applied elongation of lower jaw with distraction osteogenesis. According to our opinion, this is an exaggeration as it is proven that the development of lower jaw with a relatively fast growth will substitute at least partly the lost ground. Moreover, the surgical lengthening of the lower jaw in infancy may create significant difficulties and many complications.
Finally, in rare cases where the life of the newborn is threatened and the conservative treatment has been failed, the tracheostomy is the safest solution in order to ensure the adequate airway.